Improving Your Agency’s EMS Documentation
Now more than ever, documentation is being examined by payers using trained healthcare professionals. Since 2007, over $3.82 billion dollars has been recovered through audits and investigations. Although EMS represents a small fraction of this larger value, the government is looking to recoup every penny. The most effective way to ensure your agency is getting paid for all your services is through accurate EMS documentation.
Patient Care Report (PCR)
EMS documentation is a key component in the continuum of care. Other healthcare professionals can make important decisions that affect patient health, based on the content of a PCR. Complete your PCR as soon as time permits after a call.
The role of a PCR includes:
- Medical/QA Record
- Legal/Compliance Documents
- Basis for Reimbursement
- Source of Data Collection
Fundamentals of a PCR include:
- Demographics & Insurance
- Accurately spelled name
- Address
- DOB
- SSN
- Copy of driver’s license
- Copy of insurance card (front & back)
- Hospital face sheet
- Times
- Dispatch
- Enroute
- At Scene
- Time of Patient Contact
- Depart Scene
- At Destination
- Available
- Odometer
- At scene
- At destination
- Remember to capture fractional
- Multiple solutions available for tracking
- Narrative
- Main points of emphasis
- The detail with which you write
- The logic of how you write
How Documentation is Interpreted
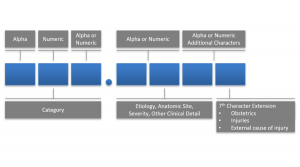
Documentation is translated into ICD-10 codes, placed on claim forms, and submitted for payment. Each character within the ICD-1- Code adds a layer of detail, while specificity helps reveal the most appropriate codes.
Everyone at Cornerstone Adminisystems is a NAAC Certified Ambulance Coder.
Fundamentals of Good Documentation
Good documentation relies on details. We created a free downloadable Documentation Quick Reference Guide that outlines the necessary items that should be included in a PCR. This information includes:

Dispatch & Response
- Dispatch
- Was it 911 or equivalent?
- If non-emergency, explain circumstances.
- Response
- Was response immediate?
- Nature of Call
- Explain if call was an emergency or non-emergency.
- Class
- Class I, II, III, IV (definitions can vary)
- Chief Complaint
- Patient’s condition as described during dispatch.
- If non-emergency, precisely explain reason for transport.
- Unit(s)
- BLS, MICU, ALS Squad
- Unit numbers
- Assisting units (often for Paramedic Intercepts)
Arrival & Assessment
- Scene Assessment
- Explain what you find.
- What’s the situation at hand?
- Initial Observations
- Your general impression of the patient, skin, eyes, breathing, is patient alert, oriented, etc.?
- For non-emergencies, does the patient meet medical necessity for use of an ambulance?
- Reported Complaint
- What the patient (or family member, witness) tells you
- Assessment
- A head-to-toe assessment
- Use mnemonics (consider explicitly explaining OPQRST reveals, AVPU reveals, etc.)
Treatment & Results
- Treatment/Interventions
- A thorough description of what you did
- Results of Treatment/Interventions
- The outcome of your treatment decisions
- How patient responded to what you did
- Packaging
- Bandaged, boarded, C-spine stabilization, straps, no straps, etc.
- How Patient Got to the Ambulance
- Walked under own power, assisted, wheelchair, stretcher, etc.
Transport/Disposition
- Transport & Ongoing Condition
- Patient’s condition enroute
- Ongoing assessment, additional interventions
- Patient’s response
- Where you are taking patient and why
- Transfer of Care
- How patient was transferred, sheet lift, log roll, hospital workers assisted, bed number
- Final Disposition
- Patient’s condition as transfer is completed.
- Refusals
- Document these to the same extent as you would a transport, be thorough, explain what you said and did.
- Protocols/Medical Command
EMS Documentation Workshop
We encourage everyone to take pride in their documentation. It reflects on the provider, the agency, and their respective standards of professionalism.
Cornerstone Adminisystems offers EMS documentation workshops to all our client partners, with in-person and virtual options available. For information on hosting a class visit EMS documentation or contact us on becoming a Cornerstone partner.


