The Coronavirus Aid, Relief, and Economic Security (CARES) Act Provider Relief Fund is part of the $178 billion distributed from the US Department of Health and Human Services to hospitals and healthcare providers on the front lines of the coronavirus response. The multiphase distributions to providers has provided much needed funding relief during the pandemic response.
If you acknowledged and accepted the terms and conditions online for the first distribution, you also agreed to the reporting requirements. Likewise, if you did not return the funds, then by default you still agreed to the terms. In a twist of fate, the terms which you agreed to when you accepted the funding has changed as of June 11th, 2021.The revised Post-Payment Notice of Reporting Requirements are available online in their entirety. Key updates include the following:
- The period of availability of funds is based on the date the payment is received (rather than requiring all payments be used by June 30, 2021, regardless of when they were received).
- Recipients are required to report for each Payment Received Period in which they received one or more payments exceeding, in the aggregate, $10,000 (rather than $10,000 cumulatively across all PRF payments).
- Recipients will have a 90-day period to complete reporting (rather than a 30-day reporting period).
- The reporting requirements are now applicable to recipients of the Nursing Home Infection Control Distribution (formally known as the Skilled Nursing Facility and Nursing Home Infection Control Distribution) in addition to General and other Targeted Distributions.
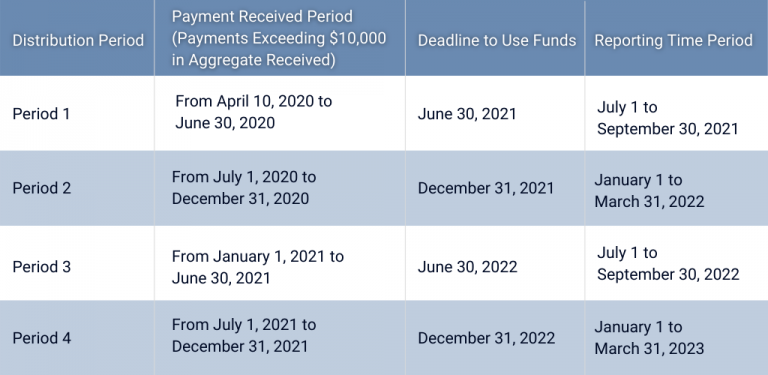
The Provider Relief Fund Reporting Portal (PRF Reporting Portal) will be open for users beginning July 1st, 2021. Portal users will be able to register and report on payments received from April 10, 2020 through June 30, 2020. We are advising our billing partners to register early and complete the reporting requirements prior to the marked deadlines. Additional deadlines based on additional distributions include the following:
Please keep in mind that it can take approximately 20 minutes to register for the PRF Reporting Portal. Additionally, the entire registration form must be completed for you to save your progress. If you are a billing partner, you will need specific payment information from Cornerstone Adminisystems (CAS). Please reach out to your Client Services representative to confirm the following information:
- “TIN (Tax Identification Number) of Entity that Received the Payment.” Unless your agency received these funds directly, this will be Cornerstone’s TIN.
- For “Mode of Payment,” select the option “Direct Deposit ACH.”
- “Settlement Date” is when CAS received the deposit.
- “Payment Amount” is the amount distributed to your agency.
We’ve received numerous questions regarding what data we think our billing partners should provide.
In our view, the answer to this depends on whether an agency performs cash or accrual-based accounting.
➔ If cash-based, then reporting net payments would make sense.
➔ If accrual-based, then reporting net charges would make sense.
In all cases, we recommend our billing partners consult with their accountants and/or legal counsel to ensure the most appropriate action.
To assist our billing partners who may be uncertain, or who don’t have immediate access to the data for their payments and/or net charges, we’ve created a report which consolidates this information into a single view, which can be found in CornerSource, our secure client portal, in the reporting section.
Should you have further questions regarding specific aspects of your reporting, please reference the CARES Act Provider Relief Fund: FAQs link. Additionally, there is a Provider Support Line available for those who need it at (866) 569-3522.
Partner With Us
Cornerstone Adminisystems is an employee-owned provider of billing, compliance, and revenue cycle management services to the EMS and medical transport community. Contact us for help improving your revenue cycle.